Rhesus D negative in pregnancy
11-minute read
Key facts
- Your 'Rhesus factor' (RhD) tells you if you have a protein known as 'D antigen' on the surface of your red blood cells.
- If your red blood cells don’t have the D antigen, your blood type is Rhesus negative.
- Being RhD negative isn’t usually a problem unless you are pregnant and your baby happens to be RhD positive — there is a mismatch in your blood types.
- If you are RhD negative and a small amount of your baby’s RhD positive blood enters your bloodstream during pregnancy or birth, it can cause an immune response called haemolytic disease of the newborn.
- If you are pregnant and have RhD negative blood, you will be offered anti-D immunoglobulin to prevent the problems that can happen because of this blood type mismatch.
What are blood types?
Everybody has one of 4 blood types (A, B, AB or O). You inherit your blood type (also called a blood group) from your parents.
These blood types are further identified as being either positive or negative. For example, your blood type can be A positive or A negative. The ‘positive’ or ‘negative’ shows your 'Rhesus factor' (RhD), which identifies if you have a protein called 'D antigen' on the surface of your red blood cells.
Around 17 in every 100 people in Australia have a Rhesus factor negative blood type.
Why is your blood type important during pregnancy?
Having RhD negative blood can be a problem if you are pregnant with a baby with RhD positive blood.
Your baby’s blood type is inherited from both parents. A baby may have a different blood type to their parents for this reason. This is normal and usually not a problem. A mismatch of blood types between a pregnant person and their baby can happen if the other parent is RhD positive. In some cases, this mismatch can be very important.
If your blood type is RhD negative, and your baby’s blood type is RhD positive, there can be problems if a little of your baby’s blood gets into your bloodstream during pregnancy or birth. This is called a 'sensitising event' and it can cause a problem in an unborn baby or newborn called haemolytic disease of the newborn. Both will be explained below.
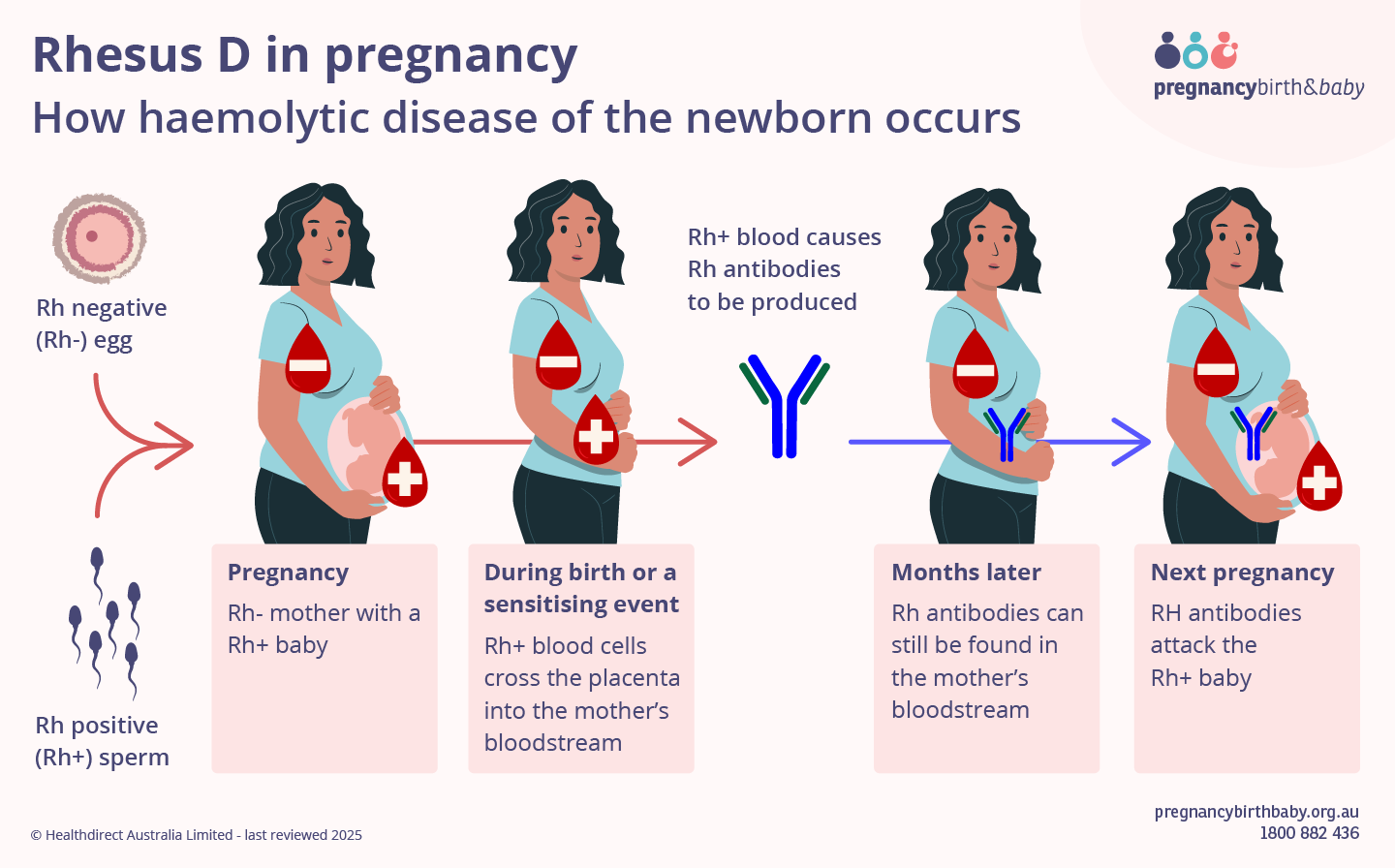
What is haemolytic disease of the newborn?
Haemolytic disease of the newborn is a condition that can happen in an unborn baby or a newborn if a small amount of your baby’s red blood cells cross the placenta into your bloodstream.
This makes your immune system react by producing antibodies to destroy your baby’s red blood cells. If these antibodies develop, they usually won’t affect your first pregnancy.
Your immune system has a good memory and can produce high levels of these antibodies if you come into contact with RhD positive blood in a future pregnancy.
This can cause serious complications for your next baby, like severe anaemia, brain damage and even death in some cases.
Because haemolytic disease of the newborn can have serious effects on your baby, preventing it is very important.
Can haemolytic disease of the newborn be prevented?
Haemolytic disease of the newborn is rare these days. This is because it can usually be prevented with injections of a medicine called 'anti-D'.
You will be offered blood tests as part of your antenatal screening, so you will be told if your blood is RhD negative or positive at the start of your pregnancy.
If you have RhD negative blood, you may be offered an injection of this medicine if there is concern that your baby’s blood may have crossed the placenta into your bloodstream. This mixing of blood is called a 'sensitising event'.
What is a sensitising event?
A ‘sensitising event’ can happen:
- during some tests you may have during your pregnancy (such as chorionic villus sampling (CVS) or amniocentesis)
- after miscarriage
- after termination (if the pregnancy is 10 weeks or more)
- obstetric haemorrhage (heavy, frequent bleeding during pregnancy)
- after an injury or accident to your abdomen (tummy)
- if your baby is in a breech position and you have an external cephalic version (where doctors turn your baby around inside your womb)
- during labour
- from an ectopic or molar pregnancy
What is anti-D?
Anti-D is an injection that contains anti-D immunoglobulin, which is a blood product made from plasma. It helps prevent Rhesus (RhD) sensitisation. It’s offered to RhD negative people during pregnancy to reduce the chance of developing antibodies against RhD positive blood.
The anti-D injection is safe for both you and your baby.
Can I find out my baby’s blood type before they are born?
Usually, the way to find out your baby’s blood type and whether they’re RhD positive is to wait until after they are born. At that time, doctors can test the blood from the umbilical cord.
Genetic screening (RhD NIPT)
A genetic screening test has been developed for pregnant women who are RhD negative, which can predict if an unborn baby will have the RhD antigen. The test is called a 'Rhesus D non-invasive prenatal test' (RhD NIPT).
It can be done starting from 11 weeks of pregnancy. This screening blood test looks at a sample of your baby’s DNA that is found in your blood, to help predict if your baby is RhD negative or positive.
This screening test has been shown to be very reliable, with more than 99% accuracy in its predictions.
Is genetic screening available to me?
Recent changes to the Medicare billing scheme have made it easier for pregnant women who are RhD negative to get this test. This means that based on the test results, only women who are pregnant with a baby that is RhD positive need to get the anti-D injections.
In Australia, there are not many people who can donate RhD immunoglobulin, which makes the supply limited.
If you are RhD negative and cannot get RhD NIPT, you will still be offered the anti-D injections, even if you don’t know your baby’s RhD status.
It’s important to know that while this test is very reliable, it’s only used to guide the use of anti-D injections. A blood test will still need to be done after your baby is born to confirm their blood type.
When might I be offered an anti-D injection?
You may be offered an anti-D injection at 28 and 34 weeks of pregnancy if your blood is Rhesus negative. If your baby’s blood is found to be RhD positive after birth, you may be offered a further dose of anti-D.
The anti-D injection may also be recommended if your doctor is concerned about you having had a sensitising event.
- If you are less than 10 weeks pregnant and have an abortion (termination), you usually don’t need anti-D. However, this may depend on your individual situation and your care needs. Always speak to your healthcare team about what is right for you.
- Anti-D should be given within 72 hours (3 days) of the sensitising event. However, it can still be given after this time.
When will I not need to get an anti-D injection?
If you have already developed anti-D antibodies in a past pregnancy you won’t need another injection in your next pregnancy. Your next pregnancies will be watched more closely than normal, and so will your baby after they are born.
There is not enough evidence to say that RhD negative women who bleed in their first 12 weeks of pregnancy need anti-D. However, if the bleeding happens again, is heavy or comes with stomach pain or serious injuries to the pelvis, anti-D may be recommended.
If you have had fetal Rhesus D (RhD) antigen screening, such as a Rhesus D non-invasive prenatal test (RhD NIPT) and your baby’s blood type is RhD negative, you might not need anti-D injections. Your midwife or doctor will talk to you about this and suggest the best way for your care.
Always speak to your doctor or midwife for advice and support if you experience bleeding during pregnancy.
Can haemolytic disease of the newborn be treated?
If your unborn baby gets haemolytic disease, it can be treated. Treatment will depend on how severely your baby is affected.
After birth, your baby will likely be admitted to a neonatal intensive care unit (a part of the hospital that specialises in taking care of newborn babies).
Treatment for haemolytic disease of the newborn after birth can include:
- light treatment (known as phototherapy)
- blood transfusions
- an injection of antibodies (intravenous immunoglobulin, also known as IVIG) to prevent red blood cells from being destroyed.
If haemolytic disease of the newborn is not treated, severe cases can lead to stillbirth or neonatal death. In other cases, it could lead to brain damage, learning difficulties, deafness and blindness. However, treatment is usually effective and these problems are uncommon.
Resources and support
If you have any questions about the risks and benefits of anti-D, or your treatment generally, speak to your doctor or midwife.
Australian Red Cross has information about haemolytic disease of the newborn.

Speak to a maternal child health nurse
Call Pregnancy, Birth and Baby to speak to a maternal child health nurse on 1800 882 436 or video call. Available 7am to midnight (AET), 7 days a week.
Learn more here about the development and quality assurance of healthdirect content.
Last reviewed: October 2025






