Eczema during pregnancy and breastfeeding
8-minute read
Key facts
- Eczema is the most common skin condition in pregnancy.
- Eczema usually gets better after you have your baby, but if you had eczema before you were pregnant, it may become worse.
- Knowing what your triggers are and avoiding them where possible can help you manage your eczema symptoms and prevent flare-ups.
- Looking after your skin health is an important part of treating eczema —using moisturiser is an important part of keeping your skin healthy.
- Most eczema treatments (including steroid creams, antihistamines and light therapy) can be used while pregnant and breastfeeding.
What is eczema?
Eczema is a skin condition where there is damage to your skin because moisture leaves your skin, making it dry and scaly. Eczema is also known as atopic dermatitis or atopic eruption of pregnancy.
It can be a long-term condition that gets better, but then comes back again later.
Eczema causes your skin to be more sensitive to irritants. It is not contagious.
What are the symptoms of eczema?
Eczema causes dry, scaly, itchy, red skin. It usually affects your face, wrists, ankles, elbow creases and the back of your knees.
Examples of eczema
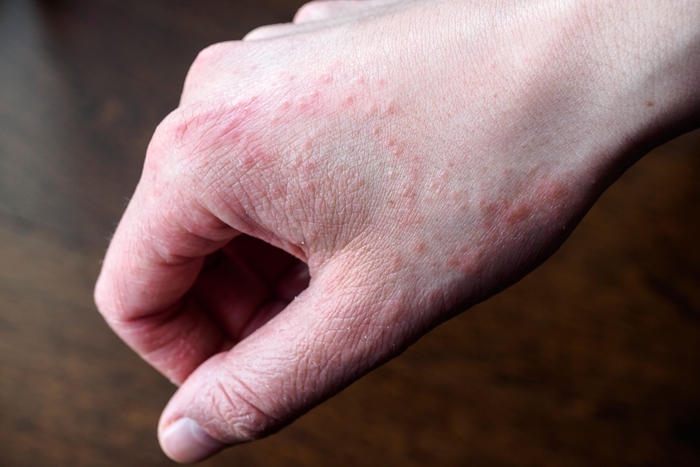
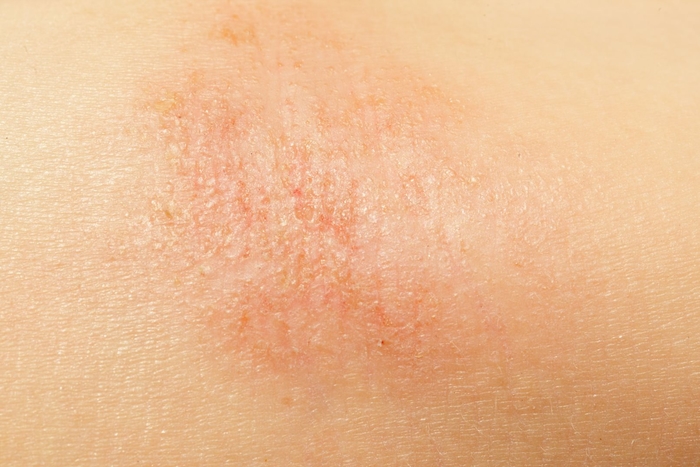
What causes eczema?
Atopy is a problem with the immune system that makes you more likely to have allergic conditions such as eczema, asthma and hayfever. People with atopy often have skin that is dry and sensitive.
You are more likely to have eczema if someone in your family has one of those conditions.
What are eczema triggers?
Eczema triggers are substances or conditions that tend to make your skin itchy, red, and irritated and cause an eczema flare-up.
Different people have different triggers.
There are some triggers you can’t avoid, such as:
- weather changes
- low humidity
- other illnesses
- stress
You may be able to avoid other triggers if they affect you. Some common triggers include:
- making your skin too hot or being in rooms that are overheated
- perfumes or scented products such as make-up, skin lotions and laundry powder
- irritating materials such as wool, polyester or acrylic in your clothes
- swimming in chlorinated pools
- house dust mite, grasses, pollens or animal dander
- washing your hands with water, soap, detergent or chemicals too often which can damage your skin’s protective barrier
Knowing what your eczema triggers are and avoiding them where possible is an important part of managing your eczema.
Examples of eczema
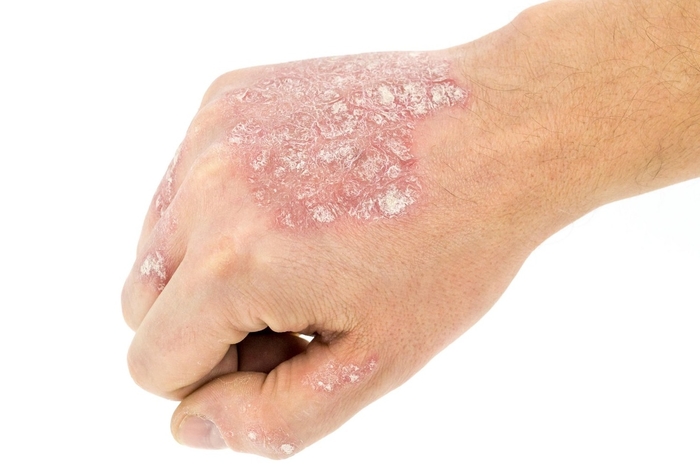

What happens if I get eczema during my pregnancy?
Eczema is the most common skin condition you can develop in pregnancy. Some people have symptoms of eczema for the first time during pregnancy, while others experience a flare-up during pregnancy. You are more likely to get eczema symptoms in the first 2 trimesters of pregnancy. If you had eczema before you were pregnant, you may notice it gets better or worse at any time during the pregnancy.
While eczema can be uncomfortable, there is no research that shows that eczema affects fertility, miscarriage, premature birth or birth differences. Your baby may be more likely to get eczema, asthma or hay fever if you or your baby’s close relatives have eczema.
How is eczema diagnosed?
Your doctor will diagnose eczema by examining your skin. They may take a small sample of your skin, known as a biopsy, to check under a microscope. Some doctors may ask you to have a blood test, which can show an increase in a protein called IgE that is associated with eczema, hay fever and asthma.
FIND A HEALTH SERVICE — The Service Finder can help you find doctors, pharmacies, hospitals and other health services.
How is eczema treated during pregnancy?
Eczema in pregnancy is treated by improving your skin health and treating the skin irritation.
You can improve your skin health by:
- having one short shower a day and not making it too hot
- using soap-free wash or bar and aqueous cream
- drying off straight after your shower by patting dry with a towel
- putting on an emollient (skin softener) once you are dry
- using a thick cream-based or ointment-based moisturiser at least twice a day to protect and improve your skin barrier
Your doctor may recommend treating your skin irritation by using:
- steroid creams or ointments over areas with eczema to reduce the redness, itch and swelling
- oral antihistamines to reduce the itch — if you are having trouble sleeping because of the itch, ask your doctor if you can use an antihistamine at night that causes drowsiness
- narrow bank ultraviolet B (UVB) phototherapy (light therapy)
- steroid tablets, if your eczema is severe
If you take other medicines to treat your eczema you should speak to your doctor to check which ones are safe in pregnancy. Do this as soon as you start planning a pregnancy or when you find out you are pregnant. Some medicines don’t have enough safety data to be used in pregnancy.
Read more on medicines in pregnancy.
Will I still have eczema after my baby is born?
If you have eczema that started in pregnancy, it will usually get better after you have your baby. You will be more likely to have eczema, asthma or hay fever in the future, and it may come back in future pregnancies.
Can I get eczema while breastfeeding?
Yes, you can get eczema while you’re breastfeeding. If you have had eczema before pregnancy sometimes your eczema will get worse after giving birth to your baby, this may mean that you have eczema while breastfeeding.
How is eczema treated during breastfeeding?
You can use emollients, steroid creams or ointments and narrowband UVB phototherapy while breastfeeding. Some medicines do not have information on their safety while breastfeeding, so it’s important you speak to your doctor or pharmacist about your options.
If you have eczema around the areola or nipple, you can apply steroid creams or ointments to this area, but it is best to put it on after you finish one feed and wipe it off gently before you feed again.
Read more on using medicines while breastfeeding.
How can I prevent eczema flare-ups?
You can prevent eczema flare-ups by avoiding triggers, such as those listed above, or those you notice for yourself. You can also follow the recommendations listed above in the treatment section to keep your skin barrier in a good condition.
Resources and support
Mothersafe has a factsheet about eczema in pregnancy and while breastfeeding. Call them on 1800 647 848 Monday to Friday, between 9am and 5pm (excluding public holidays) for advice on medicines in pregnancy and breastfeeding.

Speak to a maternal child health nurse
Call Pregnancy, Birth and Baby to speak to a maternal child health nurse on 1800 882 436 or video call. Available 7am to midnight (AET), 7 days a week.
Learn more here about the development and quality assurance of healthdirect content.
Last reviewed: September 2023



-537d5d.png)
